You may have heard about two types of coverage Medigap and Medicare Supplement. There is no difference between Medigap and Medicare Supplement Insurance. They are simply two different terms for the same type of insurance coverage offered through private insurance companies and used to cover extra health care costs not covered by Original Medicare (Parts A and B).
Extra health care costs?
That’s right, Original Medicare does not cover all of your health care costs. We’ll break it down here into the two basic parts.
Part A pays for your first 60 days in the hospital. Your share of that cost is a hospital deductible, which will be $1,484 in 2021. After 60 days consecutive days in the hospital, Medicare pays a diminishing share of your benefits. You begin paying a larger share in the form of a daily hospital copay. This can be hundreds of dollars per day, so you need supplemental coverage to protect you from those expenses on Part A services.
This can be hundreds of dollars per day, so you need supplemental coverage to protect you from those expenses on Part A services.
Part B pays for your outpatient care. This includes things like doctor visits, lab-work, imaging tests, surgeries, durable medical equipment, and even things like chemotherapy, radiation, and dialysis. After a small deductible that you pay once per year ($203 in 2021), Part B will cover 80% of all these services for you.
Your share is the other 20% of all these services, with no cap. That can be quite a bit of money for some of the bigger ticket items like surgeries or cancer treatments. You’ll need supplemental coverage to protect you from high Part B expenses.
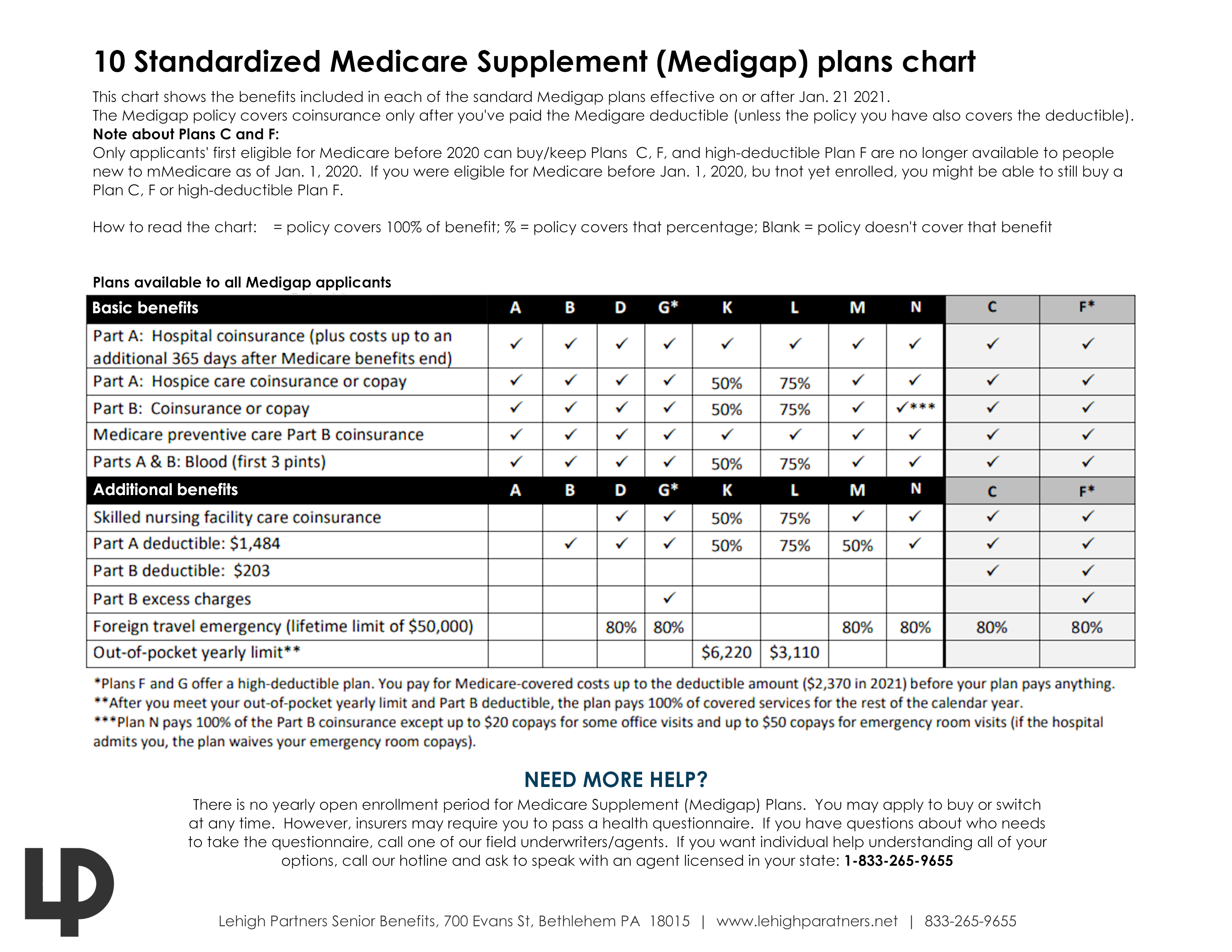
A Medicare Supplement Insurance (Medigap) policy can help pay some of the remaining health care costs, like:
- Copayments
- Coinsurance
- Deductibles
Some Medigap policies also cover services that Original Medicare doesn't cover, like medical care when you travel outside the U.S. If you have Original Medicare and you buy a Medigap policy, here's what happens:
- You pay a monthly premium to a private insurance company for your Medigap plan. This monthly premium is in addition to your monthly Medicare Part B premium.
- Medicare will pay its share of the Medicare-approved amount for covered health care costs.
- Then, your Medigap policy pays its share.
What are the types of Medicare Supplement Plans?
There are a wide range of Medicare Supplement plans. The different types of plans are named alphabetically, Plan A through Plan N. (Note, that they are not the same as other parts of Medicare, which are also named alphabetically.)
Medicare Supplement plans range from those that offer basic coverage, to those offering a much higher level of coverage. Understanding your health care needs, as well as your financial situation, can help when choosing a Medicare Supplement plan.
Compare Medicare Supplement plans online
While premium amounts differ among insurance companies, the benefits of each standard Medigap plan are the same.
For example, Medigap Plan C policies offer the same benefits regardless of which insurance company provides it. The premium amounts might be different depending on which state you live in.
Medigap plans also allow you freedom of choice in your medical care. You can see any physician or healthcare provider that participates in Medicare (nearly 900,000 providers across the nation).
Who is eligible for Medicare Supplement Insurance?
If you are age 65 or older and enrolled in Original Medicare Part B, you may be eligible to enroll for Medicare Supplement Insurance. You can apply for a Medicare Supplement plan at any time throughout the calendar year, but during your 6-month open enrollment period, you can buy any policy offered in your state and you are guaranteed coverage even if you have pre-existing health conditions.
- If you are retiring at 65 and applying for Medicare Part B, your open enrollment period lasts for 6 months starting the first day your Part B coverage begins.
- If you are not retiring until later and still getting medical coverage under your employer’s insurance, then your open enrollment starts when you do retire and sign up for Part B coverage.
Medicare Supplement plans are also available to you if you are younger than age 65 and eligible for Medicare due to disability.
You must already have or be entitled to Medicare Parts A and B before you can buy Medicare Supplement insurance.
When Can I Enroll in a Medigap Plan?
Most people become eligible for a Medicare Supplement plan shortly before age 65. The Open Enrollment Period for Medigap plans is six months before the first day of the month of your 65th birthday — as long as you also have Medicare Part B — or within six months of enrolling in a Medicare Part B plan.
During this time, you can buy any Medigap policy at the same price a person in good health pays, even if you have health issues.
Here is something to keep in mind. If you wait to apply after your Medicare supplement Open Enrollment period you will be subject to underwriting guidelines. This means coverage is not guaranteed. You can be declined for coverage or asked to pay more based on your health.
The Bottom Line about Medigap Insurance Plans
Medigap plans can give you peace of mind by reducing your out-of-pocket expenses and keeping your health care coverage affordable. It is a good idea to get rates from more than one carrier, as different insurance companies can charge different premiums for the same policy.
Our agents have been helping people new to Medicare for many years. We have already learned what is important and what isn’t. Our service is free, we will guide you through the next steps to enroll in the most suitable supplemental coverage and a cost-effective drug plan. We can help you avoid any unnecessary coverage.

